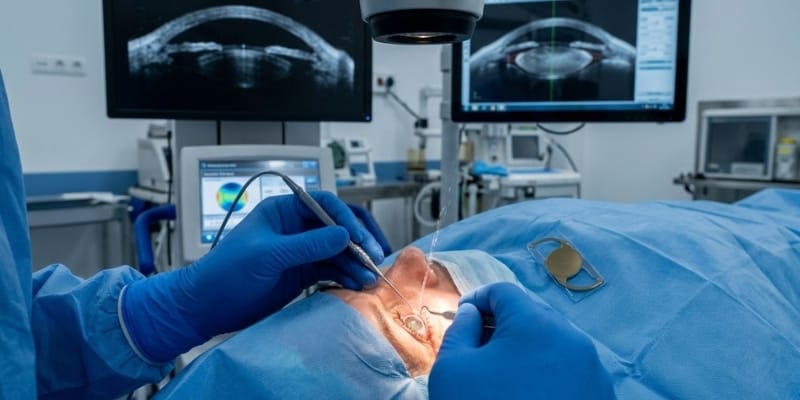
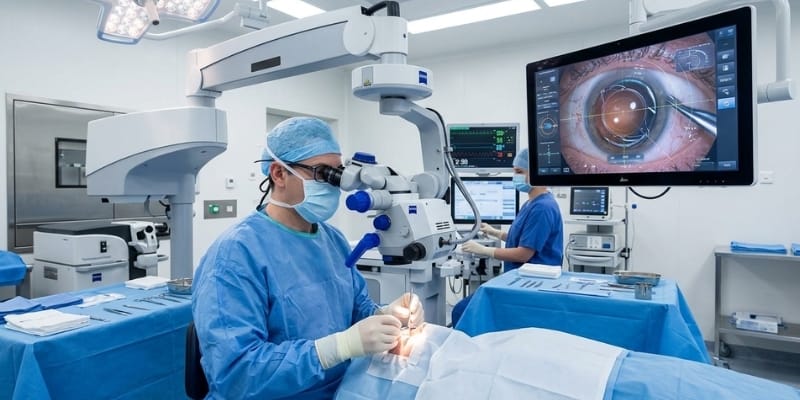
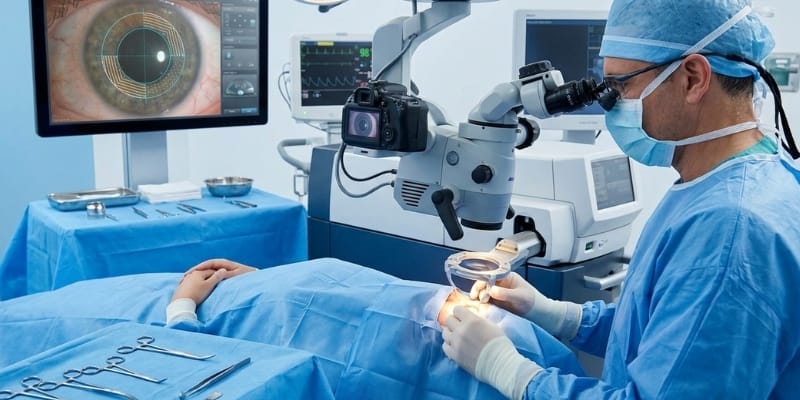
These measurements are essential to help your cataract surgeon select the proper power of the intraocular lens and give you the best vision possible after surgery.
Today you have many types of IOLs to choose from for your cataract surgery, depending on your specific needs. In addition to IOLs that correct nearsightedness and farsightedness, there are now toric.
IOLs that correct astigmatism as well.
If you don’t mind wearing glasses after cataract surgery, a monofocal lens implant usually is used. Often, only part-time use of reading glasses is needed after cataract surgery with monofocal IOLs. But if prescription eyeglasses are needed (which often is the case if you only need cataract surgery in one eye), your eye doctor typically will prescribe new glasses for you approximately one month after surgery.If you like the idea of being less dependent on glasses after cataract surgery, one way to correct presbyopia and reduce your need for reading glasses is to have your cataract surgeon adjust the power of one of your monofocal IOLs (assuming you have cataract surgery performed in both eyes) to give you a monovision correction, similar to monovision with contact lenses.
Another option is to choose one of a variety of advanced presbyopia-correcting IOLs to improve your reading vision without sacrificing your distance vision. Presbyopia-correcting IOLs include accommodating IOLs and multifocal IOLs; both types are designed to provide a greater range of vision after cataract surgery than conventional monofocal IOLs.
Be aware that not everyone is a good candidate for these premium IOLs, and choosing a presbyopia-correcting IOL will increase the out-of-pocket cost of your cataract surgery, since the added cost of these advanced lens implants is not covered by Medicare or other insurance plans.
Prior to cataract surgery, in addition to discussing the different types of IOLs, you will be advised about what to expect before, during and after your procedure. This information — which may be presented orally, in writing, via a video presentation or a combination of all three — is meant to help you make an informed decision about whether to proceed with surgery.
If you have any questions or concerns about cataract surgery, be sure to discuss them with your eye doctor and cataract surgeon prior to signing “informed consent” documents authorizing surgery.
Also, discuss with your eye doctor all medications you are taking, including non-prescription (“over-the-counter”) formulations and nutritional supplements. Some medications and supplements can increase your risk of cataract surgery complications and might need to be discontinued prior to surgery. Ask your doctor for details.